Low-income women and men were more than three times as likely to report that their health was fair or poor compared to those in the highest income group.
Thirty-five percent of low-income women aged 65 and older reporting activity limitations due to pain or discomfort.
Many people living with HIV do not receive the recommended viral load testing needed to monitor their condition.
Caesarean section rates are high – more than 1 in 4 babies who are born in Ontario hospitals are delivered by caesarean section.
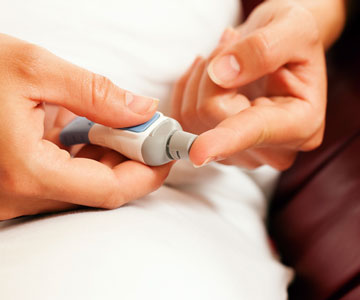
Where you live in Ontario affects a person’s risk of diabetes complications. The highest rates of complications were found in northern and rural areas of the province.
Nearly one in ten adults in Ontario have been diagnosed with diabetes. Among those with diabetes, lower-income Ontarians had more complications.
Over one-third of low-income Ontarians under age 65 with an MSK condition did not have prescription drug coverage.
Recent immigrant women were more likely than Canadian-born women to report difficulties accessing primary care.
Low-income Ontarians are more likely to have potentially avoidable hospitalizations for heart failure, chronic obstructive pulmonary disease, asthma, and diabetes.
After being hospitalized for heart failure, 20% of people were readmitted within 30 days and 59% were readmitted within one year.
Less than half of women and men in Ontario who may be experiencing depression see a doctor for this condition.
After being hospitalized for depression, one in three people did not see a physician for this condition within 30 days.
Women were more likely to have multiple chronic conditions and disability than men, while men had higher rates of potentially avoidable mortality and premature death.
The POWER Study (Project for an Ontario Women’s Health Evidence-Based Report), a multi-year project funded by Echo: Improving Women’s Health in Ontario, an agency of the Ontario Ministry of Health and Long-Term Care (MOHLTC), has produced a comprehensive provincial report on women’s health.
We examined gender differences on a comprehensive set of evidence-based indicators. We also examined differences among women associated with socioeconomic status, ethnicity, and geography. We emphasized indicators that are modifiable and can support efforts to link measures to intervention and improvement. See our Leading Health Equity Indicators.
The Report was designed to serve as an evidence-based tool to help policy makers, providers, and consumers improve the health of and reduce inequities among the women of Ontario. Educators can also use our report to teach about women’s health, health inequities, population health, and health system performance. See the POWER Health Equity Road Map.
MetaTrader 4 is a versatile trading platform widely appreciated by traders for its user-friendly interface and tools designed to enhance the trading experience. To gain access to this platform from your computer, simply download MetaTrader 4 for pc, and you'll be equipped with everything you need to analyze markets, automate trades using expert advisors, and develop your trading strategies.